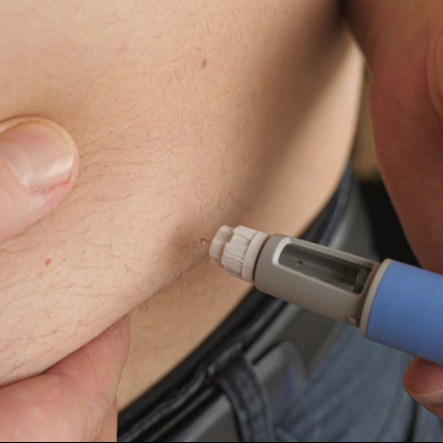
On March 23, 2023, representatives Terri Sewall (D–Alabama) and Brian Fitzpatrick (R–Pennsylvania) proposed The Resident Physician Reduction Act of 2023, a bill designed to increase the number of Medicare-subsidized medical residencies by 14,000 over seven years.
The motivation for the bipartisan bill was a desire on the part of Congress to increase the limits on physician training program funding that had been imposed by a previous act of Congress, the Balanced Budget Act of 1997, which placed caps on the number of federally funded residency slots.
The bill is expected to pass through committee, both houses of Congress, and reach the President’s desk in short order. The reason for the measure's popularity is the almost universal agreement that the US will soon face a doctor shortage.
Are We Running Out of Doctors?
The suggestion that the US faces a medical personnel crisis is not new. In fact, alarm bells have been ringing since the 1960s. There was a brief honeymoon period in the 1980s when the Council on Graduate Medical Education declared that there would probably be a physician surplus by 2000. That surplus never materialized, and calls to address the looming shortage continue until today.
A critical question must be asked: How many physicians are needed for a given population? Another crucial question is, “What do you mean by ‘physician’?” Do you mean primary care physicians like internal medicine, family medicine, and pediatric doctors? Or do you mean specialists like reproductive endocrinologists and ophthalmic (eye) surgeons? Depending on whom you ask, the answer is that primary care doctors and specialists will soon be rare.
The problem is even more complicated. There are areas of the country that are overserved by physicians (i.e., major cities) and other places where physicians are scarce (primarily rural, sparsely populated communities far from cities). On the street in Boston, there’s a measurable probability that you will bump into a physician with three medical board certifications. Meanwhile, outside Helena, Montana, you can drive for hours without passing a medical facility.
The short answer to these questions is that the US is not running out of doctors any time soon; however, the volume of calls to increase the number of physicians has continued almost unabated for over 60 years. Nevertheless, there is good evidence to suggest a maldistribution of medical professionals: Cities have too many, and rural areas have too few.

Five Reasons Why There Could Be a Doctor Shortage (and Why They’re Wrong)
A physician shortage can occur for many reasons, and the specific factors contributing to it can vary by region and healthcare system. Here are five explanations for a future physician shortage and why almost all those explanations are incomplete and flat wrong.
Population growth: An increasing population can increase demand for healthcare services, including physician services. A shortage can develop if the change in the number of physicians does not keep pace with population growth. That’s a big ‘if’. There is no reason to expect that a career in medicine will suddenly become unpopular.
Aging population: As the population ages, there is a greater need for medical care due to the prevalence of chronic diseases and age-related health issues. This phenomenon can strain the healthca
re workforce. The ‘graying of America’ is probably the most frequently advanced reason for warnings about physician shortages. American life expectancy has been rising for several generations, and decades have passed since the first time such a warning was issued; nevertheless, the anticipated physician shortage has not occurred.
Physician retirement: Many physicians are reaching retirement age, and their retirements can create gaps in the workforce. In some cases, new physicians may not adequately replace these retirements. The last of the baby boom generation (the ‘boomers’) are close to retirement age. This fact does not necessarily mean that there will be relatively fewer physicians to care for the retiring doctors.
COVID burn
out: The pandemic placed enormous burdens on all healthcare providers and health systems, and some physicians may have opted to quit. But, there have always been stresses induced by changes in the healthcare landscape. The advent of Medicare and Medicaid was accompanied by dire predictions for the end of medicine. The managed care revolution had a similar effect. The practice of medicine survived these challenges, and they will survive the pandemic as well.
Administrative burdens: Physicians often face significant administrative tasks, such as paperwork and insurance-related tasks, which can reduce the time available for patient care and contribute to job dissatisfaction. Many physicians complain that they spend most of their working hours on tasks that do not concern patient care. While this is true, it has always been thus. Before paved roads and automobiles, physicians walked (and sometimes ran) or rode horses to see patients. By comparison, modern physicians spend much more time on patient care than in the ‘good old days’.
Immigration policies: Restrictions on immigration limit the influx of international medical graduates (IMGs) who could help address shortages. This is one explanation that makes sense. The waiting list for IMGs to enter the US and practice medicine is long, and the burdens we impose on those physicians are burdensome at best and silly at worst. Most IMGs must pass the US versions of examinations they have already passed in their home countries. Most are forced to repeat residency programs they have already completed.

Five Ways to Prevent Physician Shortages
In order of priority, here are five strategies to prevent future physician shortages that don’t require Congress to allocate millions of dollars.
Reduce the barriers to entry for IMGs: With a stroke of a pen, state licensing boards could remove the requirement that IMGs sit for qualifying examinations and repeat residencies. Visa restrictions that require IMGs to return to their home countries for two years are deal-breakers for many physicians; these restrictions should be lifted.
Reduce restrictions on allied professionals: Many states are allowing nurse practitioners (NPs) and physician assistants (PAs) to work independently of the supervision of a physician. States with substantial rural populations might consider letting NPs and PAs practice unencumbered. Even if supervision would be required, the internet allows for real-time (or nearly real-time) consultations with physicians. This trend should continue.
Allow retail clinics to flourish: Pharmacy-based clinics have grown geometrically for years, and the public prefers them. There never really was a need for physician office visits for routine vaccinations and urgent care visits, and the growth of retail medicine is evidence of this fact.
Embrace telemedicine: The pandemic demonstrated that many visits and consultations can be performed safely and effectively online. Just as paved roads and cars allowed physicians to see many more patients daily, the internet has allowed providers of all types to manage many patients from a distance. Telemedicine might be one solution to the real crisis in healthcare maldistribution.
Stop tinkering! The Resident Physician Reduction Act of 2023 is necessary to undo the damage done by The Balanced Budget Act of 1997. Every act of Congress appears to generate unintended (and often expensive) consequences. A trivial example is the proliferation of Medicare and Medicaid fraud that is inevitable when gigantic programs are unleashed nationwide. Governments would be better off allowing the invisible hand of supply and demand determine how many physicians we need.
There are two constants in medicine: change and resistance to change. Nevertheless, medicine continues to change, and patient outcomes continue to improve, at least in the US. There is no reason to believe that changes in relative proportions of MD-level healthcare providers will alter that trend. The doctor may not be able to see you in the future (at least not in person), which is not necessarily bad.